Anyone who self-administers a finger-prick test to determine blood glucose levels understands that it’s not a pleasant experience. Ongoing research at the University of Bath, UK, could potentially lead to an alternative testing method.
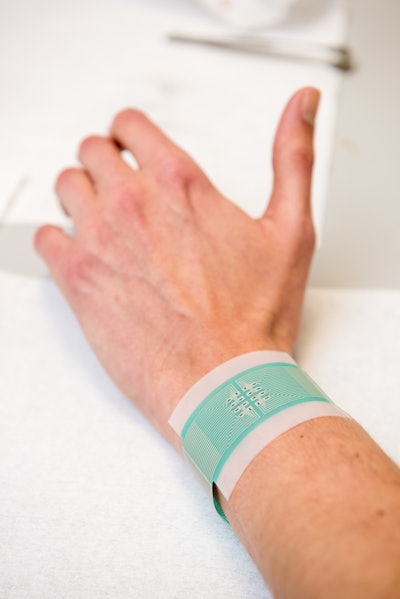
Specifically, scientists have developed a non-invasive adhesive patch that does not pierce the skin, drawing glucose out from fluid between cells across hair follicles, which are individually accessed via an array of miniature sensors using a small, safe and painless electric current. The glucose collects in tiny reservoirs and is measured.Readings can be taken every 10 to 15 minutes over several hours.
The project is a multidisciplinary collaboration between scientists from the Departments of Physics, Pharmacy & Pharmacology, and Chemistryat the University of Bath.Proof of the patch concept, says a University of Bath press release, was described in a study published in Nature Nanotechnology.
The University of Bath’s research team hopes that it can eventually become a low-cost, wearable sensor that sends regular, clinically relevant glucose measurements to the wearer’s phone or smartwatch wirelessly, alerting them when they may need to take action.
Professor Richard Guy at the University of Bath’s Department of Pharmacy & Pharmacology, says, “A non-invasive, needle-less method to monitor blood sugar has proven a difficult goal to attain. The closest that has been achieved has required either at least a single-point calibration with a classic ‘finger-stick,’ or the implantation of a pre-calibrated sensor via a single needle insertion. The monitor developed at Bath promises a calibration-free approach, an essential contribution in the fight to combat the ever-increasing global incidence of diabetes.”
Dr. Adelina Ilie at the Department of Physics, adds, “The specific architecture of our array permits calibration-free operation, and it has the further benefit of allowing realization with a variety of materials in combination. We utilized graphene as one of the components as it brings important advantages. It is strong, conductive, flexible, and potentially low-cost and environmentally friendly. In addition, our design can be implemented using high-throughput fabrication techniques like screen printing, which we hope will ultimately support a disposable, widely affordable device."
In a study the Bath team tested the patch on both pig skin, where they showed it could accurately track glucose levels across the range seen in diabetic human patients, and on healthy human volunteers, where the patch was able to track blood sugar variations throughout the day.
Since its initial development, numerous improvements have been made in the technology, according to a Bath spokesperson. That includes the ability to transmit blood glucose level results to a smartphone or smartwatch device. Researchers envision the device will be able to transmit measurements wirelessly to patients or healthcare professionals, using commercially available technology.
The next steps will include further patch design refinement to optimize the number of sensors in the array, to demonstrate full functionality over a 24-hour wear period, and to undertake a number of key clinical trials.
Will the patch be sold prescription only or over the counter? How would patches be packaged? What barrier properties would be required of the packaging to protect it in both clinical trials and ultimately for commercial production?
A University of Bath spokesperson says, “I think it’s too early to say at this stage. It will depend on several things, including the final design and manufacturing process, etc.”
One thing for certain, notes the University of Bath, is that diabetes is increasing as a public health issue. It cites World Health Organization figures that predict the worldwide incidence of diabetes to rise from 171 million in 2000 to 366 million in 2030.
A University of Bath press release notes, “An effective, non-invasive way of monitoring blood glucose could both help diabetics, as well as those at risk of developing diabetes, make the right choices to either manage the disease well or reduce their risk of developing the condition. The work was funded by the Engineering and Physical Sciences Research Council (EPSRC), the Medical Research Council (MRC), and the Sir Halley Stewart Trust.”